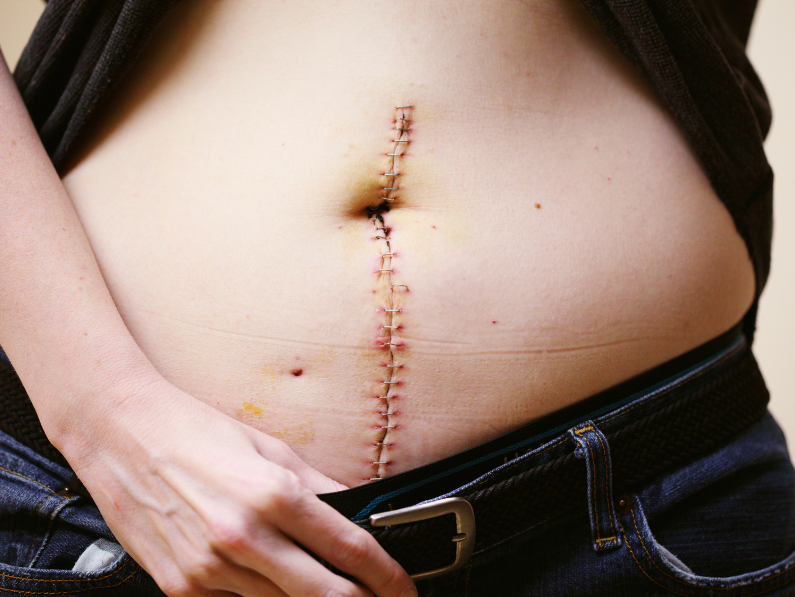
Endometriosis

How To Heal Post-Endometriosis Surgery And Feel Your Best
On a scale of one to ten, how terrified are you to undergo endometriosis surgery? Having endometriosis surgery for the first time is intimidating because you don’t know what to expect. I know I was a jumble of nerves and worried that I wouldn’t achieve any relief or...

6 Natural Solutions for Endometriosis Pain Relief
Endometriosis pain is no joke. I remember when my pain was at its worst and how debilitating it was. And since no one understood my pain, I was left to struggle alone. This led me to find natural solutions for endometriosis pain relief that could help me get some of...

Healthy Living with Endometriosis How to Improve Your Quality of Life
Healthy living with endometriosis is not impossible. But it does require some work. The primary goal is to manage chronic pain and decrease inflammation. Luckily you can make fundamental changes to your daily routine and accomplish a better quality of life. Learning...

10 Informative Endometriosis Facts You Need to Know for Increased Awareness
How much do you know about endometriosis? Unfortunately, when it comes to endometriosis facts, you probably know very little, if anything at all. But since endometriosis affects one in ten women of reproductive age, it's vital to learn more about this misunderstood...

The Truth About Getting an Endometriosis Diagnosis Helpful Info You Must Know
Getting a proper endometriosis diagnosis can be challenging. It took eighteen years and a severe health complication before receiving my official diagnosis. However, I didn’t understand the diagnostic process. And I didn’t understand how to advocate for myself...

A Simplified Definition of Endometriosis and Its Impact On My Life
What in the world is endometriosis? Perhaps this is a question that’s running through your brain. And the answer is simple yet complex because endometriosis affects everyone differently. That’s why the best way for me to define what endometriosis is will be to share...

Self Acceptance with Invisible Illness Secrets on How To Love Yourself
Cultivating self acceptance with invisible illness is tough. Learning how to love yourself when your body and mind are determined to tear you apart from the inside out is an overwhelming challenge that I wish on no one. But that’s what makes self-love and acceptance...

The Truth About Endo Risks and Complications Post Surgery And What I’m Dealing With
Endo has contributed to various risks and complications to my health post-surgery. And it makes me feel like my battle with endometriosis will never be over. While I haven't experienced the pain and severity of symptoms, I did pre-surgery. I now have conditions and...

Helpful Endo Surgery Prep Tips That Make Life Easier
Endo surgery prep can be hard to manage alone. You're already anxious and nervous about the surgery and the outcome. So, trying to remember the steps necessary to properly prepare for surgery can be overwhelming. This is why it's essential to not go through this alone...
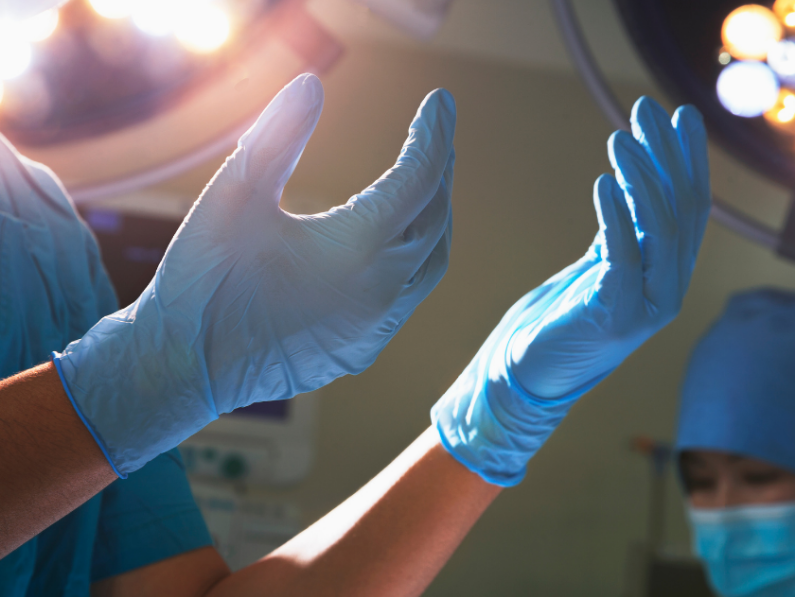
Laparotomy And Laparoscopy Differences And Similarities That’s Important To Know
Laparotomy and laparoscopy are two similar yet dramatically different surgical procedures. If you’ve landed on this article, you’re trying to figure out one of two things. The first being why your doctor recommended one over the other. The second reason is you've...