Upon finding out that I would need a laparotomy, I was instantly scared. I hadn’t heard anything about a laparotomy with all the research I had done into endometriosis and various treatments. I’d only learned about laparoscopy and its minimally invasive approach after watching videos on YouTube of multiple women sharing their experiences. So, I was utterly ignorant about what a laparotomy was. Yet, despite my ignorance, laparotomy has a similar success rate as laparoscopy. And it focuses on the same end goal. Which is to diagnose and treat underlying conditions that contribute to various painful symptoms. In my case, my surgeon wanted to determine if my ovarian cysts were cancerous or not and if I had endometriosis as was suspected. Now, if you’re similar to me and have NEVER heard about laparotomy and treating endometriosis. We’re going to talk more about this particular surgical procedure and the purpose it serves in diagnosing and treating endometriosis.
Page Contents
But First…What Is A Laparotomy?
An exploratory laparotomy is a major surgical procedure in which an incision is made on the abdomen. This incision allows access to the abdominal cavity and allows the surgeon to investigate its organs. This allows the surgeon a clear view of the reproductive organs, intestines, kidneys, bladder, spleen, appendix, stomach, liver, and pancreas. Consequently, they’re able to determine underlying conditions causing chronic pelvic pain, abdominal pain, ovarian cysts, or other complications. It’s only during surgery that they can inspect the organs and identify if injury, disease, or abnormal growths are the root cause. In many cases, a biopsy will be required to rule out cancer. Additionally, if growths related to endometriosis are found, and the surgeon is qualified to perform excision surgery, they will remove them.
In my particular situation, my surgeon was able to identify that the large cysts on both of my ovaries were not cancerous and, indeed, caused by endometriosis. Additionally, he found the presence of endometriosis on my peritoneum(tissue lining the abdominal wall and covering the abdominal organs), adhesions that glued my left fallopian tube and ovary to my intestines, a corpus luteum cyst, as well as two uterine fibroids.
Ok, So How Does It Differ From A Laparoscopy?
When it concerns the procedure itself, the end goal is the same. Which is to find and identify if symptoms are caused by an underlying issue. The two factors that differentiate the laparotomy from the laparoscopy are the incision required and the recovery process.
Larger Incision
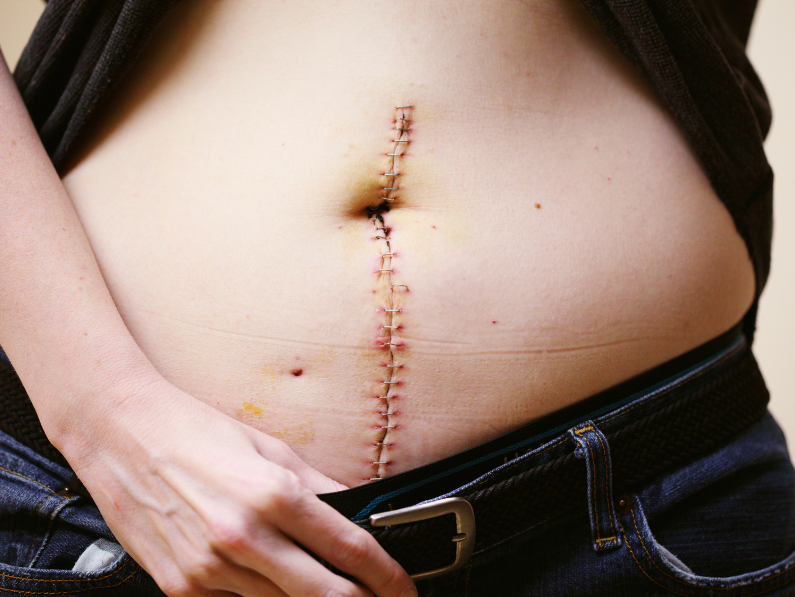
The laparotomy is an open surgery, be prepared to have a larger incision. It will either be vertical (from the middle of the sternum to the top of the pubic bone) or horizontal (the bikini line). This, of course, depends on your health condition and situation and will vary from person to person. Additionally, your incision will require some form of stitches or staples to close it. And a longer healing time is to be expected. There will be special instructions for you to follow regarding adequately caring for your incision to minimize infection risk. Additionally, depending on how your body heals, you may have a scar.
It’s almost been one-year post-surgery, and I still have a visible scar from my incision. It has improved slightly, and in many ways, I still feel like it’s becoming less noticeable, but it’s still visible.
Longer Recovery Time
Since the laparoscopy is minimally invasive, you may not need an extended stay in the hospital. And, you will not require as much time to recover. However, with a laparotomy, you will need to spend some time in the hospital and have a more extended recovery period. The length of your hospital stay and recovery will vary according to your health and what procedures were performed.
I had 4 different procedures that consisted of a myomectomy (fibroid removal), cystectomy(removal of chocolate cysts and corpus luteum cyst), unilateral salpingo-oophorectomy(removal of left ovary and fallopian tube), and excision surgery (endometriosis tissue cut out of peritoneum and adhesions removed. I remained in the hospital for three days and was released on the fourth day. And it took me six weeks to reach a functional level and a full six months to get back to normal.
When Is A Laparotomy Indicated?
I’m not a doctor or medical professional, so I can’t say “if” and “when” you will need a laparotomy. Since some various factors and conditions can lead to your surgeon recommending this procedure for you. However, I can share two of the significant reasons the laparotomy was recommended for me.
The first reason had to do with the size of my cysts. I had a 17 cm cyst on my left ovary and a 13 cm cyst on my right ovary. Consequently, the size of the cysts had not only caused a multitude of symptoms, but my abdomen was swollen and distended. Which was awkward because it looked as though I was in my second trimester of pregnancy. Secondly, my blood tests revealed an elevated level of cancer antigen 125. Which meant there was a possibility that the cysts were cancerous, and I was at an increased risk of having ovarian cancer. I talk more about the CA125 in more detail in another blog post, which you can find here. However, my surgeon felt an exploratory laparotomy would be the best option due to these issues’ complexity.
Preparing for Surgery & Recovery
Your pre-op and post-op instructions are going to depend on what procedures your doctor performs, your unique health, and what your doctor recommends for you. When they schedule your surgery, there will be a pre-op appointment in which your vitals are recorded, and you’re administered a blood test. At this time, the nurse will most likely provide you with literature detailing the steps you are to take to prepare for your surgery and what to expect afterward. Additionally, you should share any medications or supplements you’re currently taking and follow the instructions on when to discontinue the use of these medications. If there are any questions or concerns, this is the perfect time to share them with your nurse. What’s most important is that you should feel comfortable and confident as you prepare for your surgery.
During my pre-op appointment, my nurse was amazing and explained what I needed to do to prepare for my surgery. She instructed me to discontinue taking my supplements, naproxen sodium, ibuprofen, and aspirin 5 days before my surgery. We also discussed what to eat the day before surgery and when I should begin fasting. I wasn’t required to do a bowel prep, but I did have to cleanse with a unique cleanser the evening before and the morning of my surgery. And, I wasn’t allowed to put lotion, perfume, or any type of cosmetic or personal care product on my body. I was even required to remove my nail polish. Knowing these things in advance helped me understand what I needed to do to prepare for my surgery. Furthermore, knowing in advance what my recovery would entail helped my husband and I plan ahead.
Providing Some Context
As I mentioned initially, I didn’t know much about the laparotomy when it was first discussed with me. Mostly because laparoscopy is performed in the majority of situations. Due to this, there will be more information and first-hand experiences detailing it on the internet and social media. For the small few who may have to undergo a laparotomy as I did, I wanted to share what I learned and offer some general insight, so you don’t feel alone.
However, it’s essential to keep in mind that my experience may differ from yours. Everyone’s endometriosis journey is going to be different and unique to that person. This is why it’s so essential you discuss everything with your doctor. Make sure you understand fully the procedures they’re recommending and ask questions, so you’re clear on what’s going on and what to expect.
Additional Resources
Very Well Health: Exploratory Laparotomy
Healthline: What Size is Normal for An Ovarian Cyst






Thanks for your post, Kat. I also just went through a laparotomy and am in the recovery stage now. It’s tough. I appreciate all the information.
Praying for your recovery and glad that you found the post helpful!
Thanks so much for sharing. I’m recovering from a Laparotomy to remove a tumour/my right ovary and Fallopian tube, and I haven’t found any other first hand experiences online.
You’re welcome! I hope your recovery process is going well.